Ironman Journey – Blog 3
/in Articles, cycling, Massage, Running, Training, Triathlon training, Uncategorised, Wellness/by Pete TangIronman Journey – Blog 2
/in Articles, cycling, Running, Training, Triathlon training, Wellness/by Pete TangIronman Journey – Blog 1
/in Articles, cycling, Running, Training, Triathlon training, Wellness/by Pete TangThe Rest & Recovery Menu
/in Articles, Massage, Physiotherapy Advice, Rehabilitation, Running, Strength, Training, Triathlon training, Wellness/by Pete TangHow can process goals help you return to hobbies & sports
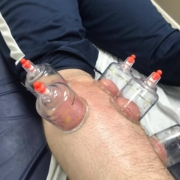
/in Articles, cycling, Golf, Physiotherapy Advice, Rehabilitation, Running, Triathlon training, Wellness/by Pete TangWhat is Cupping?
/in Articles, Massage, Rehabilitation, Running, Training, Triathlon training, Warm-Ups & Stretching, Wellness/by Pete TangPre-Event Sports Massage
/in Articles, Massage, Physiotherapy Advice, Running, Training, Triathlon training, Warm-Ups & Stretching, Wellness/by Pete TangRun analysis episode 3… Foot placement
/in Articles, Physiotherapy Advice, Rehabilitation, Running, Training, Triathlon training/by Pete TangGet in Contact
We understand that people often don't know what we do or how we can help. Don't worry we're here to help.
To ask us a question or to book an initial appointment simply call 01454 54 00 66 for our Bristol Clinic or 01291 76 99 66 for our Chepstow Clinic and one of our friendly team will assist you with your enquiry.
Alternatively, please fill in the form on the Contact page.
View More TestimonialsTrustindex verifies that the original source of the review is Google. After struggling for a year with debilitating lower back pain, chronic sciatica and being post-partum, Kate Moore (physio) has helped me tremendously. She has built not only my strength back but also my confidence through her detailed, caring and passionate support. She understands the challenges of everyday working/family life and helped me integrate the rehab into that.Trustindex verifies that the original source of the review is Google. I booked in for a running analysis. Pete did a really comprehensive assessment on my recurrent ankle issues and explained things in a lot of detail to help me understand the underlying reasons for my injuries. He gave me the confidence to try running again and equipped me with the knowledge to prevent further injuries. I have seen running specialists / physios / podiatrists in the past but I felt this was the best assessment I’ve had yet. Thanks!Trustindex verifies that the original source of the review is Google. The Physio Clinic was very helpful when I thought I had sciatica. Craig found out what the problem was and gave me advice as well as exercises to do at home. Booking sessions was straightforward.Trustindex verifies that the original source of the review is Google. Saw Pete Tang at the clinic about a knee injury I'd had for a year, which another physio had struggled to properly diagnose or help with. Got a detailed diagnosis on my first visit in June along with an evolving exercise programme and was improving within a month and able to run a half marathon within three. Pete was knowledgeable, friendly and helpful and went through more advanced treatment options if the injury didn't respond – but did not push these and after three sessions told me I was good to go unless things worsened. Highly recommended – thanks!Trustindex verifies that the original source of the review is Google. I was very happy with the treatment I received from Dave and would definitely recommend.Trustindex verifies that the original source of the review is Google. Just had a neck and shoulder sports massage with Luke—highly recommend! He quickly found the problem areas and used the perfect pressure to release tension. I noticed a big difference straight away and felt so much better after. Luke is friendly, professional, and clearly knows his stuff. Would definitely book again!Trustindex verifies that the original source of the review is Google. I had three months of physiotherapy with Dave Mercy starting in June 2025 to help rehabilitate my right foot following a medically necessary operation to break and re-position my heel bone following a diagnosis tibialis posterior tendinopathy with a split tear. The physiotherapy started approx three months after surgery. Dave helped me to progress from being in an air-cast boot on my first visit and unable to put my weight through my foot, onto massages to reduce and eventually eradicate the post surgical swelling in my foot, onto a range of exercises in the gym to exercise, stretch and strengthen my foot and allow me to complete everyday activities that I can now once again enjoy. The support that Dave provided was comforting in the early days and then as the gym exercises progressed, Dave was encouraging and challenged me to develop my foot strength, flexibility, and gave me the confidence to put my full weight through my foot and complete a wide range of exercises that I didn’t think would be possible. I am walking well and whilst the finer aspects of my foot recovery will take longer to achieve, for now I can walk without the pain I previously had, which is a massive achievement. Thanks Dave, you had a hugely positive impact on my level of recovery!Trustindex verifies that the original source of the review is Google. Excellent service, very quick to get me an appointment. Katie did a very good massage on my back and calves - I feel better already :-)Google rating score: 4.9 of 5, based on 282 reviews